Help the person make an informed choice about whether to make an advanced care plan. It should be entirely their decision. An advance care plan can cover areas such as the person’s thoughts on different types of care, support or treatment, financial matters, and how they like to do things (for example shower rather than bath).

The NHS Route to Success series (now archived) was a series of guides which assists GPs to tailor care for different groups of individuals based on their personal circumstances. Holistic needs assessment for patients (formerly known as the SPARC tool) Discussion paper about helping GPs to identify end of life patients and plan ahead.

You can also write down your wishes in a document that is sometimes referred to as an advance statement or, in Scotland, anticipatory care plan. Writing down your wishes can make it easier for people to understand them and follow them in the future. It’s your choice whether you make an advance care plan.

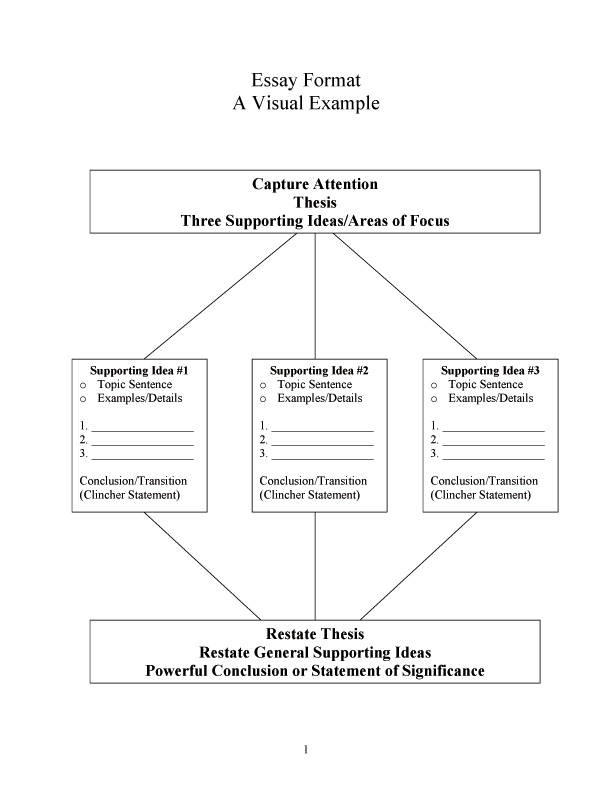
Care Plan Template and Completed Example Care Plan. The Care Plan Template is provided for your reference as a starting point for the documentation that you should have in place as a provider of care and support services. Please also see worked Example Care Plan for information.